Eczema: My Lived Experience as an Aesthetic Nurse (And What Finally Helped)
- luminateaesthetics
- Apr 7
- 4 min read
If you’ve ever struggled with eczema, you’ll know it’s not “just a skin condition.” It’s physical, emotional, and at times completely overwhelming. As an aesthetic nurse of 10+ years, I thought I understood skin. But nothing prepared me for experiencing eczema myself.
This is my honest story—from first symptoms to diagnosis, the mistakes I made, and what’s finally starting to work.
When It All Started…
At 30, after having my first baby, I began noticing flare-ups in random places—starting on my neck. At first, I brushed it off. Even with my medical background, I didn’t immediately recognise it as eczema.
After multiple GP visits, I was eventually diagnosed with “general eczema” affecting my neck and arms. I was prescribed a strong topical steroid and told to return if it didn’t improve.
It did… slowly. I managed it. I moved on.
Or so I thought.
Postpartum Flare-Ups: When It Got Severe
After my second baby, everything changed.
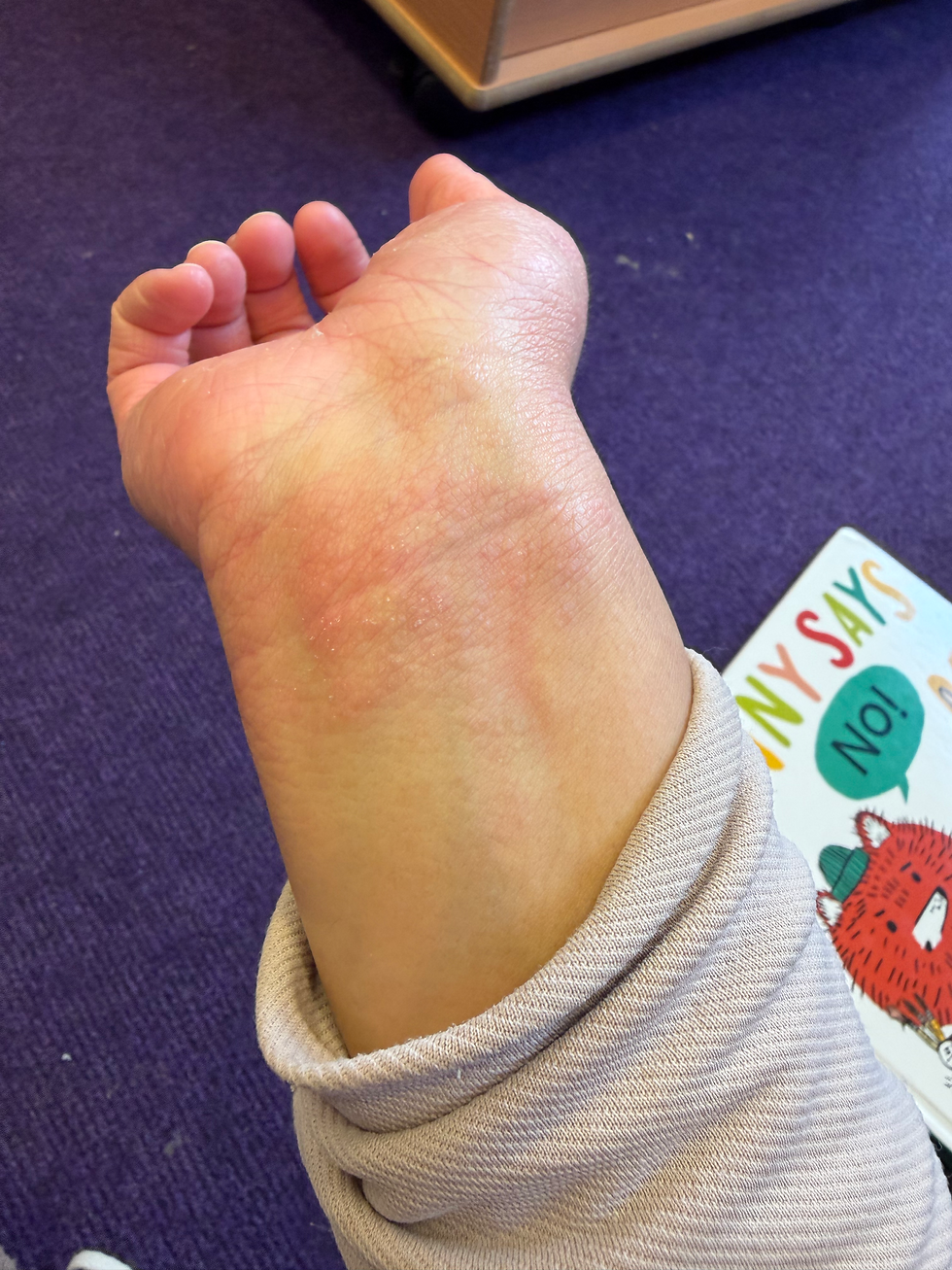
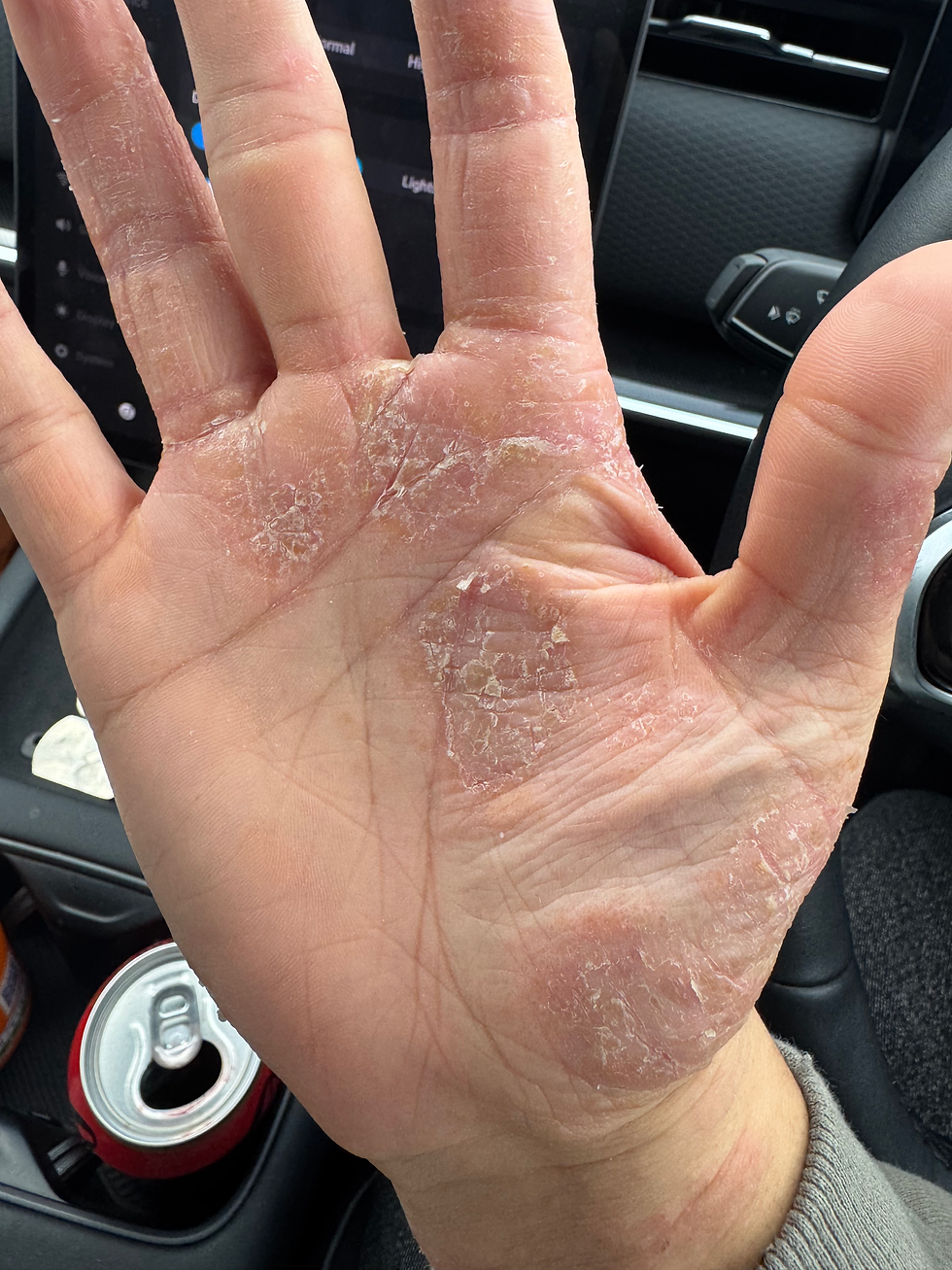
My skin flared like never before—especially on my hands. As someone who works with their hands every day, this wasn’t just uncomfortable… it was debilitating.
I was later diagnosed with:
Seborrheic eczema
Pompholyx (dyshidrotic eczema)
If you’ve had pompholyx eczema, you’ll understand the itch. It’s relentless. You scratch, blisters form, they burst… and suddenly your hands are swollen, cracked, and too painful to even straighten.
It’s exhausting. And honestly, quite isolating.
The Steroid Cycle (And Where It Went Wrong)
Like many people, I was repeatedly prescribed topical steroids.
They worked… temporarily.
But within days, my skin would become:
Paper-thin
Extremely sensitive
More painful than the original flare
Then the cycle would repeat.
The worst moment came when I had a severe flare on my face—around my eyes and mouth—five months postpartum. Out of desperation, I used the steroid I’d been given.
Big mistake.
It caused immediate burning and left me with open, damaged skin on my face. That was a turning point.
Finally Seeing a Dermatologist
Frustrated and feeling unsupported, I decided to go private.
That consultation changed everything.
I received a formal diagnosis and, importantly, clarity:
I had been prescribed the wrong type of steroid
It was too strong, especially for my face
It contained an antibiotic I didn’t need
Instead, I was prescribed:
Tacrolimus (Protopic) – a non-steroidal immunosuppressant to control inflammation
A safer, lower-potency steroid for short-term flare-ups
Advice to manage a yeast overgrowth contributing to my symptoms
My treatment plan also included:
Regular diluted antiseptic baths to restore skin balance
Medicated shampoo (like ketoconazole-based formulas) for seborrheic eczema
Using targeted treatments beyond just steroids
For the first time, I felt like I had a plan.
Progress… Then Setbacks
Things improved—briefly.
But flare-ups kept coming back. My hands were constantly painful, and mentally, I was drained.
I tried everything:
Dietary changes
Hormonal contraception (suspecting a hormonal trigger)
Endless creams and emollients
Nothing gave consistent, long-term relief.
Even on holiday in Thailand, I couldn’t enjoy the pool—chlorine triggered instant flare-ups despite rinsing. It affected everything.
Hitting a Wall with Treatment
Back home, I pushed for further support—but was initially told I hadn’t completed all treatment steps for a referral.
That was incredibly frustrating.
I was prescribed another strong steroid (Dexamethasone) and told to try again.
This time, I approached it differently:
I focused treatment on my hands
I aimed to control the “core” flare area
Interestingly, when my hands improved, the rest of my skin followed.
That changed my mindset.
A More Balanced Approach
At my follow-up, my GP was much more supportive. Together, we created a plan to gradually step down steroid strength rather than rely on long-term high potency use.
This included:
Transitioning from Dexamethasone → Beclometasone → (hopefully) milder options
Combining steroids with tacrolimus
Consistent, frequent moisturising
It hasn’t been easy—but I’m finally seeing progress.
What’s Currently Working for Me
After trying everything, these are the products I personally keep going back to:
Wild Mint “Calm Balm” – great for calming irritation without heaviness
I also:
Moisturise every 30 minutes (hands - body at least twice a day)
Apply creams immediately after washing
Use cotton gloves overnight for better absorption
Sea salt bathes (twice a week if possible)
Changed the brand of gloves to 'Zero Nitrile gloves' from 'Physique'
And importantly—I avoid overly greasy products that interfere with daily life (because realistically, compliance matters).
The Emotional Side No One Talks About
I didn’t fully understand how much a skin condition could affect mental health… until I lived it.
Eczema can impact:
Confidence
Work
Sleep
Daily comfort
If you’re going through it right now—feeling frustrated, exhausted, or like nothing is working—I truly understand.
And you’re not alone.
Where I’m At Now
I’m currently in the process of reducing steroid strength gradually, with the goal of maintaining control through:
Consistent moisturisation
Intermittent tacrolimus use
Minimal steroid reliance
For the first time, that feels realistic.
Final Thoughts
Eczema isn’t one-size-fits-all. What works for one person may not work for another—but persistence, the right guidance, and understanding your triggers can make all the difference.
If you take anything from my story, let it be this:
Don’t ignore persistent symptoms
Don’t be afraid to seek a second opinion
And don’t underestimate the impact this condition can have
I’ll continue to share updates as I (hopefully!) keep improving.
If you’ve made it this far—thank you for reading 🤍













Comments